Indigeous people, according to the 2017 general census, a total of 43,378 individuals, or 1.2% of the total population of the Republic of Congo, were mainly distributed in three departments: Likouala, Sangha, and the Lékoumou. They are among the most deprived social categories in terms of the rights to survival, development, protection and participation, notwithstanding the existence of an arsenal of administrative and structural provisions existing at the institutional level, supposed to constitute a major asset for the promotion of the rights of these populations. In reality, indigenous people remain poor, marginalized and vulnerable. Malnutrition mainly affects indigenous children (40% compared to 26% of the general population) and pregnant women. This is one of the causes of infant morbidity and mortality (250/00 compared to 117/00 for the general population).
An Efficient Approach to Support Vulnerable Populations
In order to get as close as possible to the beneficiaries, the approach consists of finding and taking charge of the target populations of the project by focusing resources and energies on their places of residence: two workshops, one of which one per health district allowed the prioritization of areas; health, then localities and villages were organized with community participation as the first steps. The descents of community relays in these localities with a form developed to identify all vulnerable people were then organized. Finally, the mobile or advanced teams organized targeted visits to these localities after having obtained a firm meeting with the community leaders for the targeted offer of care.
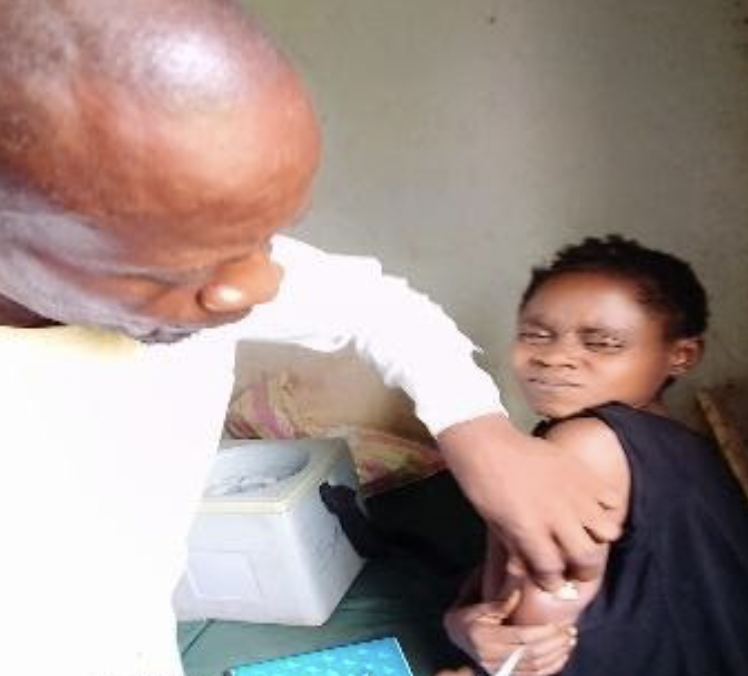
Marie (last name omitted to protect identity), one of these women and mother of twins, received in Prenatal Consultation (ANC) during a mobile outing organized as part of the project. She explained the reasons for the conflict with the vaccination schedule of her twins: “It has often been difficult for me to go to the health center because of the amounts to pay for care. If the care is free, I will come and I will bring the children whenever I or the children are sick". Marie is not the only case. Indeed, the fixed, mobile or advanced activities organized in 2020 within the framework of the project allowed the following results:
- 235 Prenatal consultations (ANC) were conducted, with 29% completed by indigenous women
- 491 Vitamin A and folic acids supplements of 979 expected (50% of the target) in women
- 794 cases of moderate and severe malnutrition were detected out of 9,860 screenings carried out (i.e. 8% of cases)
- 493 doses of yellow fever vaccine administered, including 144 to indigenous children (representing 29% of cases)
- 13,959 children aged 12 to 59 months dewormed
- 1,226 doses of the polio vaccine (1, 2, 3) administered including 451 to indigenous children (37%)
- 1,226 doses of Penta 1, 2 and 3 were administered including 451 to indigenous children (i.e. 37%)
- 1,156 doses of RR1 and 2 were administered, including 347 to Aboriginal children (i.e. 30%)
- 749 doses of Rota 1 and 2 weread ministered, including 290 to indigenous children
- 491 A vitamin A supplements out of 979 expected (i.e. 50%)
Free Healthcare for the Most Vulnerable
To remove financial barriers to healthcare for the most vulnerable, a mechanism has been set up to ensure free referral and counter-referral for all vulnerable indigenous and Bantu populations, consisting in providing transport between the community and the health center and another from the health center to the referral hospital, if applicable, and the cost of the food ration.

On the left, two natives taken care of within the framework of the project:

- One received a free cesarean section for pre-eclampsia
- The other benefited from a safe delivery in the health center during a descent for mobile, advanced and fixed strategies




















